Penicillin Allergy: Symptoms, Risks, and Why a Medical Alert Bracelet Could Save Your Life

Penicillin Allergy: One of the Most Commonly Reported Drug Allergies in the World
Penicillin allergy is the most frequently reported drug allergy, with approximately 10% of the global population believing they are allergic to penicillin or related antibiotics. However, research has revealed a surprising truth: according to the Centers for Disease Control and Prevention (CDC), fewer than 1% of the population is truly allergic to penicillin, and more than 90% of people who report a penicillin allergy can actually safely tolerate the drug.
Despite this, a penicillin allergy label — whether confirmed or unconfirmed — has significant medical implications. People labelled as penicillin-allergic are given alternative antibiotics that are often broader-spectrum, more expensive, and associated with more side effects and antibiotic resistance. For those who genuinely are allergic, exposure to penicillin can trigger reactions ranging from mild rashes to life-threatening anaphylaxis. This is why understanding your allergy and wearing a medical alert bracelet is so critically important.
Understanding Penicillin and Penicillin-Type Antibiotics
What Is Penicillin?
Penicillin, discovered by Alexander Fleming in 1928, was the first antibiotic and remains one of the most important drugs in medical history. It belongs to the beta-lactam family of antibiotics, which kill bacteria by disrupting their cell wall synthesis. Penicillin-type antibiotics include:
- Penicillin V and Penicillin G: The original forms, still widely used
- Amoxicillin: One of the most commonly prescribed antibiotics worldwide
- Ampicillin: Used for a wide range of bacterial infections
- Flucloxacillin: Commonly prescribed for skin infections
- Co-amoxiclav (Augmentin): Amoxicillin combined with clavulanic acid
- Piperacillin: Used for serious infections, often in hospital settings
If you are allergic to one penicillin-type antibiotic, you are generally considered allergic to all of them.
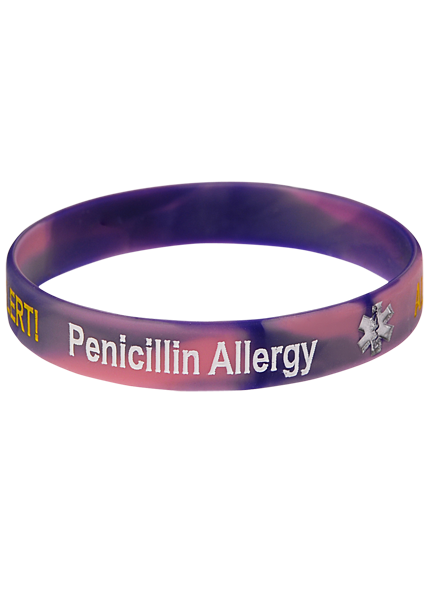
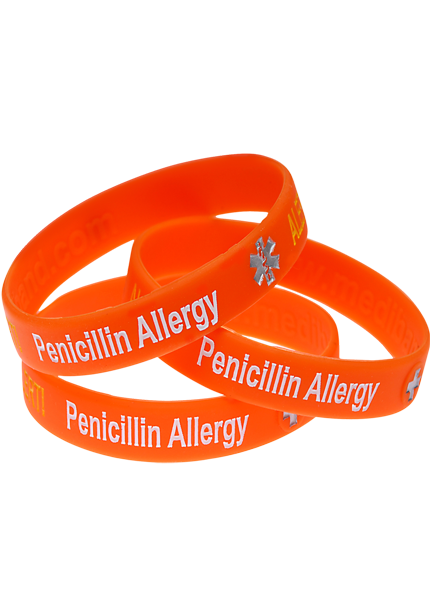
Penicillin Allergy Medical Alert Bracelets
Clearly warn healthcare providers about your penicillin allergy in any emergency.
Symptoms of Penicillin Allergy: From Mild to Life-Threatening
Mild to Moderate Reactions
Most penicillin allergy reactions are mild and occur within hours of taking the medication:
- Skin rash: Red, itchy, raised bumps (hives/urticaria) — the most common reaction
- Itching: Generalised itching without a visible rash
- Swelling: Localised swelling, often around the face, lips, or eyes (angioedema)
- Fever: Low-grade fever that develops during or shortly after treatment
Severe Reactions: Anaphylaxis
In rare cases, penicillin allergy can cause anaphylaxis — a severe, potentially fatal allergic reaction that requires immediate emergency treatment. Anaphylaxis affects approximately 1-5 per 10,000 courses of penicillin treatment. Symptoms develop rapidly (within minutes) and include:
- Difficulty breathing: Throat swelling, wheezing, or tightness in the chest
- Severe drop in blood pressure: Causing dizziness, lightheadedness, or loss of consciousness
- Rapid or weak pulse
- Nausea, vomiting, or diarrhoea
- Widespread hives and flushing
- Confusion or a sense of impending doom
Anaphylaxis requires immediate injection of adrenaline (epinephrine) and emergency medical care. Without treatment, it can be fatal within minutes.
Cross-Reactivity: Other Antibiotics to Watch Out For
One of the most important aspects of penicillin allergy is cross-reactivity with other antibiotics, particularly cephalosporins. Cross-reactivity means that the immune system reacts to a structurally similar drug even though it is not penicillin itself.
- Cephalosporins: First-generation cephalosporins (such as cephalexin) have the highest cross-reactivity rate, estimated at 1-2% in people with confirmed penicillin allergy. Later generations have lower risk but should still be used with caution.
- Carbapenems: Such as meropenem — historically thought to have significant cross-reactivity, but recent evidence suggests the actual risk is very low (less than 1%)
- Monobactams: Such as aztreonam — generally considered safe for penicillin-allergic patients
Always inform your doctor, dentist, and pharmacist about your penicillin allergy so they can choose appropriate alternative antibiotics and avoid potentially dangerous prescribing.
Should You Get Tested for Penicillin Allergy?
Penicillin Allergy Testing
Given that over 90% of reported penicillin allergies are not true allergies, allergy testing is highly recommended. Penicillin skin testing, followed by an oral challenge under medical supervision, is the gold standard for confirming or excluding a penicillin allergy.
Why get tested? De-labelling a false penicillin allergy has major benefits:
- Access to first-line antibiotics that are more effective and have fewer side effects
- Reduced risk of antibiotic-resistant infections from alternative antibiotics
- Lower healthcare costs
- Better surgical infection prevention (penicillins are preferred pre-surgical antibiotics)
However, until you have been formally tested and cleared, you should always treat your allergy as genuine and ensure it is clearly communicated to every healthcare provider you encounter.
Why a Penicillin Allergy Medical Alert Bracelet Could Save Your Life
For anyone with a confirmed or suspected penicillin allergy, a penicillin allergy medical alert bracelet is one of the most important things you can wear. Here is why:
- Emergency situations: If you are unconscious, confused, or unable to communicate after an accident, illness, or allergic reaction, your bracelet tells medical teams not to administer penicillin or related antibiotics. This prevents a potentially fatal allergic reaction on top of your existing emergency.
- Hospital admissions: During hospital stays, multiple healthcare professionals may be involved in your care. A visible bracelet serves as a constant reminder that is impossible to miss, even when medical notes are not immediately available.
- Dental procedures: Antibiotics, including amoxicillin, are commonly prescribed before and after dental procedures. Your bracelet ensures your dentist or oral surgeon is immediately aware of your allergy.
- Travel safety: When travelling internationally, language barriers can make communicating allergies difficult. The universal medical alert symbol on your bracelet is recognised by healthcare professionals worldwide.
- Children: If your child has a penicillin allergy, a bracelet ensures teachers, coaches, camp leaders, and emergency responders can protect them when you are not there. The penicillin allergy pack provides bracelets for multiple settings.
A study in the Journal of Allergy and Clinical Immunology: In Practice (2020) found that drug allergy errors are among the most common preventable adverse events in hospitals. A clearly visible medical alert bracelet is the simplest and most effective way to prevent penicillin being administered to someone who is allergic.
Living with a Penicillin Allergy: Practical Tips
Managing a penicillin allergy is straightforward once you take the right precautions:
- Wear a medical alert bracelet: The most important step you can take — shop the full range
- Inform every healthcare provider: Doctors, dentists, pharmacists, and hospital staff should all have your allergy on file
- Carry an allergy card: Keep a written record of your allergy in your wallet alongside your medical ID bracelet
- Know your alternatives: Discuss suitable alternative antibiotics with your doctor in advance so you have a plan if you develop an infection
- Consider allergy testing: If your allergy was diagnosed in childhood or you have not been tested formally, talk to an allergist about penicillin skin testing
- Teach your children: If your child has a penicillin allergy, ensure they can articulate their allergy to adults and always wear their medical ID bracelet
Penicillin allergy is manageable with the right knowledge and precautions. Whether your allergy is confirmed or suspected, wearing a medical alert bracelet ensures that in any medical situation — planned or emergency — healthcare providers are immediately aware of this critical information. It is a simple step that provides powerful, round-the-clock protection.
Frequently Asked Questions
How common is penicillin allergy?
Approximately 10% of the global population reports a penicillin allergy, but the CDC confirms that fewer than 1% are truly allergic. Over 90% of people labelled as penicillin-allergic can safely tolerate the drug. Many childhood allergies resolve over time. Formal allergy testing through skin tests and oral challenges can confirm or exclude a genuine allergy.
What are the symptoms of a penicillin allergy?
Mild reactions include skin rash, hives, itching, localised swelling, and low-grade fever, typically appearing within hours of taking the medication. Severe anaphylaxis — affecting about 1-5 per 10,000 courses — causes breathing difficulty, severe blood pressure drop, rapid pulse, widespread hives, and potential loss of consciousness, requiring immediate adrenaline injection.
Can penicillin allergy cause anaphylaxis?
Yes. Although rare (approximately 1-5 per 10,000 penicillin courses), anaphylaxis is a life-threatening allergic reaction that develops within minutes. Symptoms include throat swelling, breathing difficulty, dangerous blood pressure drops, and loss of consciousness. Without immediate adrenaline injection and emergency care, anaphylaxis can be fatal, making a medical alert bracelet essential.
Why should someone with a penicillin allergy wear a medical alert bracelet?
In emergencies when you cannot communicate — after accidents, during severe illness, or during allergic reactions — a medical alert bracelet prevents healthcare providers from administering penicillin or related antibiotics. Drug allergy errors are among the most common preventable hospital adverse events. A visible bracelet provides constant, unmissable protection wherever you go.
If I have a penicillin allergy can I take other antibiotics?
Most alternative antibiotics are safe, but cross-reactivity exists with some drugs. First-generation cephalosporins have a 1-2% cross-reactivity rate with penicillin. Later-generation cephalosporins and carbapenems carry lower risk. Always inform your doctor about your penicillin allergy so they can choose appropriate alternatives and avoid potentially dangerous prescribing.