Lymphedema Bracelet: Why It Could Save Your Life
What Lymphedema Is — and Why It Quietly Becomes a Medical Emergency
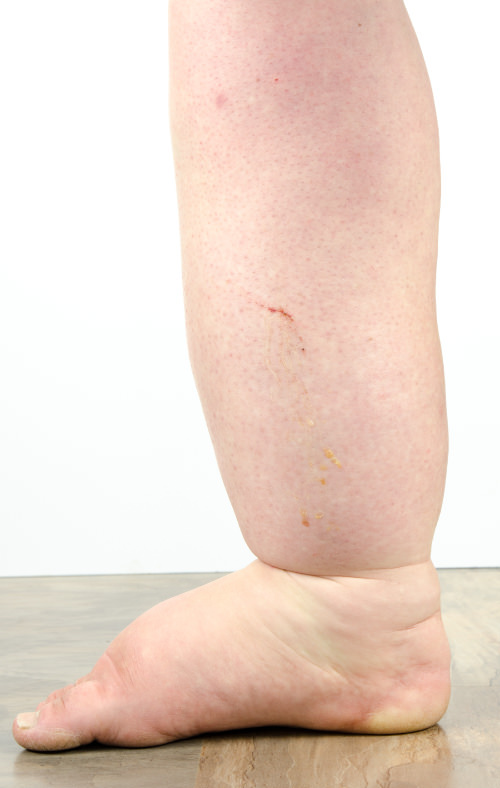
Lymphedema is the chronic swelling of an arm, leg, or other body part caused by a disrupted lymphatic system. The lymphatic system normally drains fluid out of tissues; when it's damaged — by surgery, radiation, infection, or congenital factors — fluid pools and the limb swells, sometimes dramatically. It affects an estimated 200 million people globally, most commonly arising after breast cancer treatment, gynecological surgery, melanoma surgery, or filariasis in tropical regions.
For people living with lymphedema, the swollen limb is more than a daily nuisance. It's also a clinical-decision flag every time the person walks into a hospital, GP clinic, dental surgery, or emergency room. The wrong treatment in the affected limb can trigger painful flare-ups, severe infection, or permanent worsening of the condition. A clear medical alert bracelet on the affected limb is the most reliable way to stop those mistakes from happening.

The Specific Risks a Lymphedema Bracelet Prevents
Most general clinicians know what lymphedema is in theory. In practice — especially during busy ER shifts, dental visits, or routine clinics — the affected limb can easily be treated like any other limb unless something flags it. The bracelet does that.
Blood Pressure Cuff on the Affected Arm
Compression from a blood pressure cuff can trigger acute swelling, pain, and prolonged flare-up. Lymphedema patients are advised to NEVER allow BP measurement on the affected limb. A clearly visible "LYMPHEDEMA — DO NOT USE THIS ARM" bracelet stops a nurse mid-action, every time.
IV Insertion or Injection in the Affected Limb
Same principle. Needle sticks, cannulation, and injections into a lymphedematous limb increase infection risk and can worsen the condition. The bracelet directs cannulation to the unaffected side instead.
Blood Draws on the Affected Limb
Phlebotomy on a lymphedema arm carries similar risks. The bracelet is the simplest defence — a phlebotomist who reads "LYMPHEDEMA" on the wrist redirects the blood draw without question.
Cellulitis and Infection
Lymphedematous limbs are highly susceptible to cellulitis — bacterial skin infection that can spread quickly and require IV antibiotics. The bracelet alerts ER staff to take infection seriously, prioritise wound cultures, and consider lymphedema as a complicating factor in management.
Surgery and Anaesthesia
Pre-operative checklists in major hospitals include lymphedema screening, but it's easy to miss in elective day-surgery clinics or rural facilities. The bracelet ensures positioning, BP cuff placement, IV access, and post-op compression all account for the affected limb.
Shop Lymphedema Medical Alert Bracelets
Visible alerts that protect the affected limb during routine care, surgery, and emergencies.
Who Develops Lymphedema?
Lymphedema is broadly grouped into two types:
Primary Lymphedema
Caused by congenital lymphatic-system malformations. Often appears in childhood, adolescence, or young adulthood. Genetic conditions like Milroy disease and Meige syndrome fall into this category.
Secondary Lymphedema
The more common form, caused by damage to a previously normal lymphatic system. Major causes:
- Breast cancer treatment — surgery (axillary lymph node dissection or sentinel node biopsy) and radiation are the leading cause in developed countries.
- Gynecological cancers — surgery and radiation to pelvic lymph nodes can cause leg lymphedema.
- Melanoma surgery — sentinel and complete lymph node dissection in arms or legs.
- Filariasis — a parasitic infection endemic in tropical regions; the leading global cause of secondary lymphedema.
- Trauma or chronic infection — repeated cellulitis or significant injury to lymphatic pathways.
According to HealthDirect, lymphedema is one of the most under-recognised long-term complications of cancer treatment, with a significant proportion of cases going undiagnosed in the first year.
What to Engrave on a Lymphedema Bracelet
The most useful lymphedema medical ID is short, action-relevant, and unmistakable. Five priority fields:
- Wearer's name
- "LYMPHEDEMA" alert prominently
- Affected limb — "LEFT ARM" or "RIGHT LEG" — critical for clinical decisions
- "NO BP / IV / NEEDLE" — explicit instruction to clinicians
- Emergency contact phone number
For people who travel internationally or live in non-English-speaking environments, multilingual or QR-coded bracelets help. The QR code links to a fuller profile that translates the warning into the local language and lists current treatments, garments, and specialist contact.
Choosing the Right Bracelet for Daily Wear
Lymphedema bracelets are worn 24/7 — including in the shower, during compression-garment use, and overnight. Material and fit matter:
Pink-Toned Silicone
Soft, waterproof, easy to update with a permanent pen if instructions change. Pink is the recognised colour for lymphedema awareness — visible and instantly recognisable to nurses and paramedics.
Engraved Stainless Steel
Polished, durable, and dressy. Engraving stays sharp for years. Best for stable cases where the affected limb and instructions don't change.
Designer Reversible
One side discreet (everyday look), the other side a clear medical alert. Useful for people who want a low-profile look outside clinical settings but a clear alert when they enter a hospital, GP, or dental clinic.
Wallet Card or QR-Coded Band
Pair with a wallet card carrying treatment plan, lymphedema therapist contact, compression-garment specs, and recent surgical history. The QR-coded band scales this — any phone can scan and see the full profile in seconds.
Living with Lymphedema — Beyond the Bracelet
Wearing a medical alert is one part of long-term management. The full plan typically includes:
- Specialised compression garments — bandaged or fitted sleeves/stockings that prevent fluid pooling.
- Manual lymphatic drainage — gentle massage technique performed by a trained therapist.
- Daily skin care — careful moisturising, watching for cuts and insect bites that can trigger cellulitis.
- Targeted exercise — pump-action movement of the affected limb to support drainage.
- Healthy weight management — body weight directly affects lymphedema progression.
- Regular review with a lymphedema therapist — typically every 3-6 months in early management, less often once stable.
The bracelet is the always-on layer that protects the work the rest of the plan does. Without it, one accidental BP cuff or IV stick can undo months of careful self-care.
Frequently Asked Questions
Why is a medical alert bracelet so important for lymphedema?
Because lymphedema is invisible until it flares, and the wrong routine action — a blood pressure cuff, IV insertion, blood draw on the affected limb — can trigger pain, infection, or permanent worsening. The bracelet alerts every clinician at every visit, every time, before they reach for the limb.
What should I engrave on a lymphedema medical alert bracelet?
Five essentials: your name, "LYMPHEDEMA" alert, affected limb (LEFT ARM, RIGHT LEG), explicit "NO BP / IV / NEEDLE" instruction, and emergency contact. Pair with a wallet card carrying treatment plan, lymphedema therapist contact, and surgical history.
Should the bracelet go on the affected or unaffected limb?
On the affected limb. The whole point is that anyone reaching for that limb sees the warning before they act. A loose-fitting silicone band that doesn't restrict circulation is the safest material — never tight enough to compress.
Can I wear a lymphedema bracelet with a compression garment?
Yes — pick a slim, soft material that fits comfortably under or over the compression sleeve. Silicone bands are particularly compatible. Make sure the bracelet is visible to clinicians during procedures even when the garment is on.
Are lymphedema bracelets just for cancer survivors?
No — anyone with lymphedema benefits, regardless of cause. Primary (congenital) lymphedema, post-surgical, post-radiation, post-trauma, and filariasis-related lymphedema all create the same daily clinical risks. The bracelet protects equally in all cases.















I Have a pace maker !!